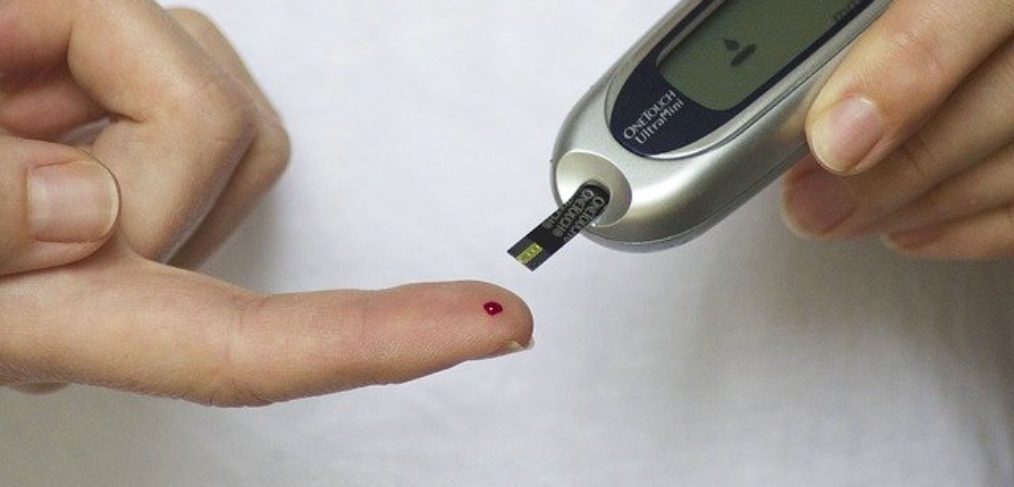
Almost no one becomes pre-diabetic suddenly. The onset is progressive. But unless you know the signs, a diagnosis might blindside you. Your lab work might appear “normal” one year, then be over the limits the next.
The Pre-Diabetic Evolves Over Years
Shouldn’t the main question we ask be, ‘Why is this happening?’ instead of ‘What new drug can we find to treat it?’ – Dr. Mark Hyman
Unfortunately, when a doctor gives an unexpected or diagnosis, we want a quick fix. But there are no sudden reversals any more than there are sudden pre-diabetics. The choices that lead to a pre-diabetic outcome are decades in the making! They begin with high-stress, low-nutrient lives, deprived of sleep, and filled with numbing recreation and damaging toxins.
Today, there are probably 100 million Americans with pre-diabetes. However, 90% of them don’t realize it! Because they haven’t been diagnosed yet. But the cycle is the same.
There are pressures. Relationship woes, work deadlines, unmet expectations, and a race to be good enough. You hit the ground running when the alarm goes off. IF you grab breakfast, it’s a “muffin and a mocha.” You work through lunch – or munch on chips and coke. Then you snarf a chocolate bar or an energy drink to get you through the afternoon slump. You put in extra hours to get the job done and have a voracious appetite by the time you eat dinner at 8 p.m. After the pizza, you wrangle with the kids and their homework, the laundry, and the rest of the to-do list. Finally, after bedtime has come and gone, you slump into a recliner to watch a movie while you snack on popcorn.
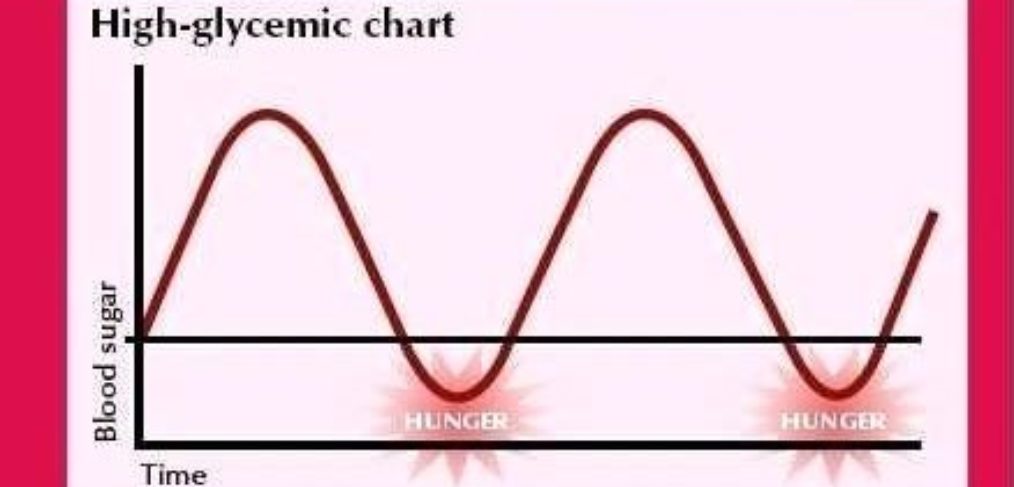
The stress alone, without any of the junk food, would be enough to catapult you into pre-diabetes. Stress increases blood sugar by design! If you have to fight a saber-tooth tiger, you need quick energy. So, your body converts glycogen stores from your liver and muscle tissue into quick fuel. Next, you start craving. Can you see why? Your body wants more and more fast energy, and it needs to replenish its stores. As a result, you eat more high-glycemic foods. As stress hormones remain high, your sleep tanks! And you become more fatigued and sedentary.
Progression from “Normal” to “Sick”
If we were to put you, the “sudden pre-diabetic” under a historical microscope and examine your life, we would see several distinct stages of change happening over a period of years.
First, as characterized above, you simply have too much stress. Living the modern lifestyle, you exhibit no abnormal blood markers or indicators of inflammation… yet. But you might see the scales reflecting a 10-pound weight gain. If you characterized your diet, it would be more than 50% refined carbohydrates. In fact, you would be consuming the perfect storm of inflammatory fats, low-fiber foods, and an excess of chemical additives and preservatives.
Second, you begin to have episodes of hypoglycemia: blood sugar crashes! Why? Because at this point insulin levels are so consistently high and your cells are becoming so “deafened” to insulin’s message, the fuel cannot get into your cells. Your cellular energy crashes because you are “insulin resistant.” You have to be grazing on snacks all through the day to avoid brain fog, anxiety, irritability, shakiness, and headaches. You might even be drinking a lot of caffeine to stave off headaches and to keep the fatigue at bay. Your stress hormones spike when your blood sugars crash, which sends cravings skyrocketing. You begin to accumulate a little more belly fat, and a lab test might show triglycerides climbing.
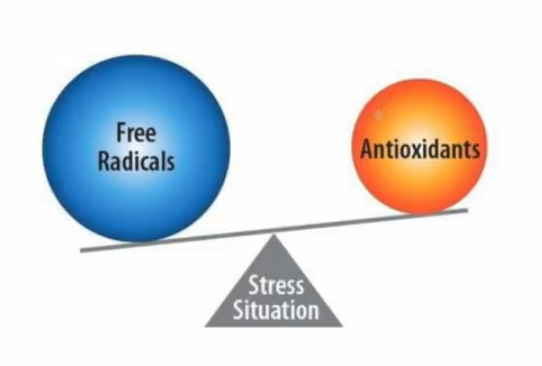
Third, some lab markers begin to show up now. Your fasting glucose levels rise above 85 and your c-reactive protein (a marker of inflammation) may be slightly over normal lab ranges. Your organs and tissues, over-exposed to high glucose, begin to show signs of oxidative stress – if you’re looking! You might start having signs of gall bladder disease, heart or kidney disease, or changes to your vision. If a doctor is very astute, he might diagnose you with Non-Alcoholic Fatty Liver Disease (NAFLD).
Finally, you match the criteria for metabolic syndrome: high triglycerides, low HDL, high blood pressure, and abdominal obesity. Your arteries are forming plaque, and you may have high levels of homocysteine. Your blood sugars are at last consistently high enough to be measured in terms of a Hemoglobin A1c test over 5.7. Suddenly, you are pre-diabetic.
Suddenly Not Pre-diabetic?
Diagnosing pre-diabetes as the first sign of disease is like waiting for a raging house fire to engulf the second story before you decide to buy a smoke detector. – Tracy Harrison, founder School of Applied Functional Medicine
Your retreat from disease will be as dramatic as your lifestyle changes. If you make moderate changes, you’ll likely still end up with diabetes; it just won’t progress as quickly.

So what striking approach should you use? Intermittent fasting, keto, vegan, or perhaps a combination?
What seems to make the most difference is lifestyle changes supported by low-glycemic whole foods. Not all carbohydrates are created equal. You want to choose ones that are not dense, like grains, and that are not quick-absorping, like juice. The lightest, slowest carbs are seeds and non-starchy vegetables.
Here’s a quick checklist of lifestyle considerations:
- Choose unrefined, clean, whole foods. Remove all products made with flour.
- Break the habit of needing foods to be sweetened.
- Anchor your diet with vegetables, building up tolerance to fiber gradually.
- Hydrate with pure water. Break the habit of self-medicating with caffeine or alcohol.
- Eat natural fats liberally, but emphasize whole foods and unrefined olive oil.
- Eat enough protein: at least 15 grams for breakfast and 50 for the daily total.
- Move. Daily. Get your heart rate up doing something you enjoy at least every other day.
- Rejuvenate. Prioritize sleep, and choose activities that increase your gratitude and joy.
- Work with a qualified practitioner to use targeted supplements to re-sensitize your cells to insulin and increase your antioxidant capacity.